Oral health is essential for every person’s well-being, whether adult or child. In your role as a parent, your children’s dental health can be a main concern. The state of a child’s teeth often influences their happiness. From ensuring that they can eat and speak properly to easing their anxieties based on looks, a parent’s […]
Blog
What to Do When You Have a Dental Emergency
Dental emergencies happen. You play sports and crack a tooth. You go on vacation and a crown falls out. Or how about a migraine-inducing toothache? You need some quick action to deal with an emergency. But when the dental office is closed or your regular dentist is far away, it can feel like you’re facing […]
Why Do My Root Canalled Teeth Still Hurt?
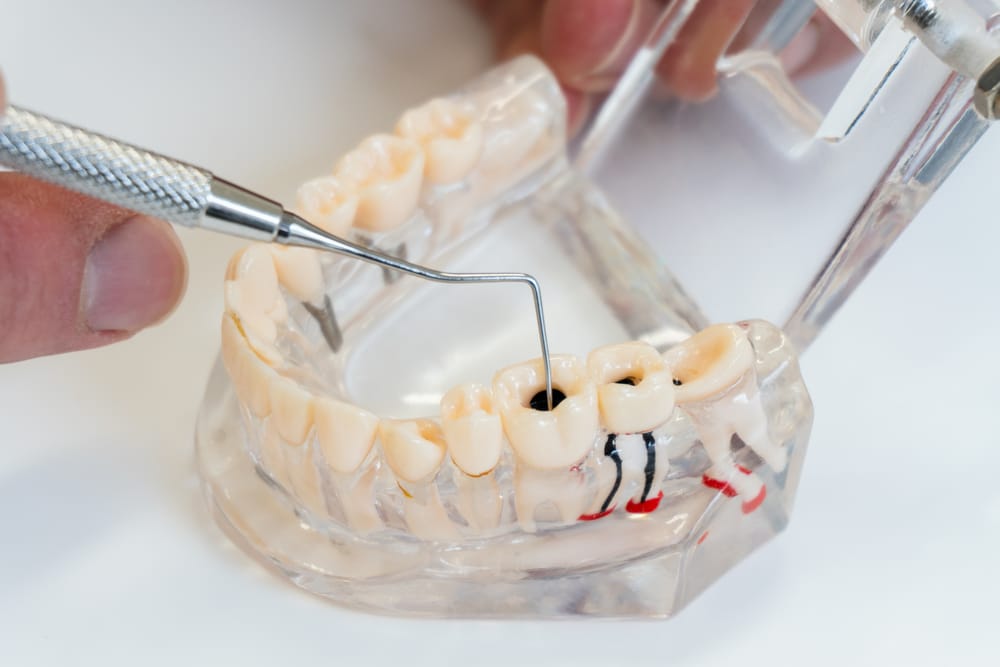
Undergoing a root canal is a common solution to alleviate severe tooth pain caused by infection or damage to the dental pulp. However, for some patients the question may arise: “Why do my root canaled teeth still hurt?” While rare, there are some people who continue dealing with infection and pain after a root canal. […]
Why Do My Teeth Hurt When the Weather Changes?
Have you ever experienced pain when it rains or snows? At Taylor Dental, we often come across some rare dental anomalies such as; “Why do my teeth hurt when the weather changes?” If you’ve ever experienced tooth sensitivity or discomfort during shifts in temperature, you’re not alone. Today we’ll explore the common reasons behind weather-related […]
How Cosmetic Dentistry Enhances Your Overall Oral Health
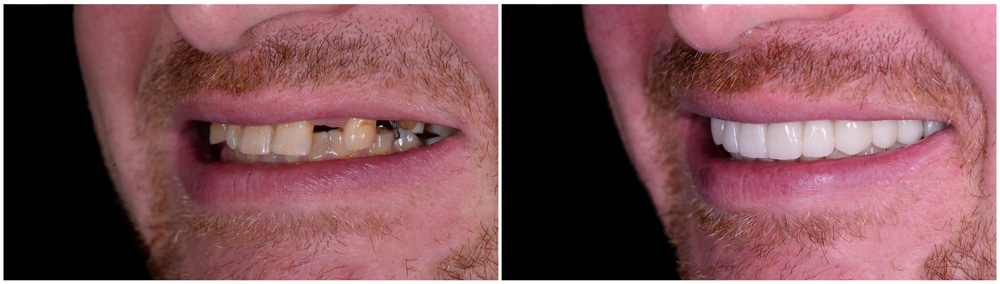
Cosmetic dentistry may focus on making your teeth look better, but its applications are far greater than that. These procedures have gained importance in the past years because they can significantly affect oral health. Let us look at how they perfect your smile and improve your health and overall lifestyle. Improved Oral Hygiene One of […]
Why Annual Dental Check-ups Are Essential for Your Smile
Maintaining a healthy and radiant smile involves more than regular brushing and flossing at home. Regular dentist check-ups are essential for oral health care, offering several benefits beyond a pretty smile. Let’s delve into why scheduling and attending your dental examinations is good for the longevity and well-being of your teeth and gums. Preventive Care […]
Dental Health and Overall Wellness: The Surprising Connection
The pursuit of health and wellness is not a single-faceted endeavor. Instead, overall fitness is achieved by making daily and consistent decisions contributing to your health and well-being. One of those decisions is taking care of your oral health. Your mouth is one of the main entry points in your body. It’s how the body […]
Orthodontic Marvels: A Comprehensive Look at Braces and Invisalign
In the field of orthodontics, technological advancements have created several treatment options for those who want straighter, more aligned teeth. Conditions that create the need for orthodontic intervention include malocclusions (such as overbite, underbite, crossbite, and underbite), irregular spacing, misalignment, crowded teeth, and impacted teeth. This post will look at orthodontic therapy and two technological […]
The Smile Experts: Unveiling the Role of Dentists in Your Oral Health
You might not realize it, but your dental health significantly impacts your health in general, increasing the importance of proper dental care throughout your life. However, many factors contribute to why there might be inconsistency in receiving dental care, including not feeling comfortable with your dental team. At Taylor Dental, we understand the issues surrounding […]
Beyond the Chair: A Closer Look at the Comprehensive Dental Services Offered
Choosing a dental team that offers a wide range of dental services can significantly affect your oral health, overall health, and how confident you feel about your smile. This all-around approach to dental care has many perks beyond regular cleanings and checkups. It allows you to truly get to know your team and feel comfortable […]











 Call Us: 406.652.9204
Call Us: 406.652.9204  Email Us: office@taylorcosmeticdental.com
Email Us: office@taylorcosmeticdental.com Visit Us: 2700 Grand Ave STE E, Billings, MT 59102
Visit Us: 2700 Grand Ave STE E, Billings, MT 59102